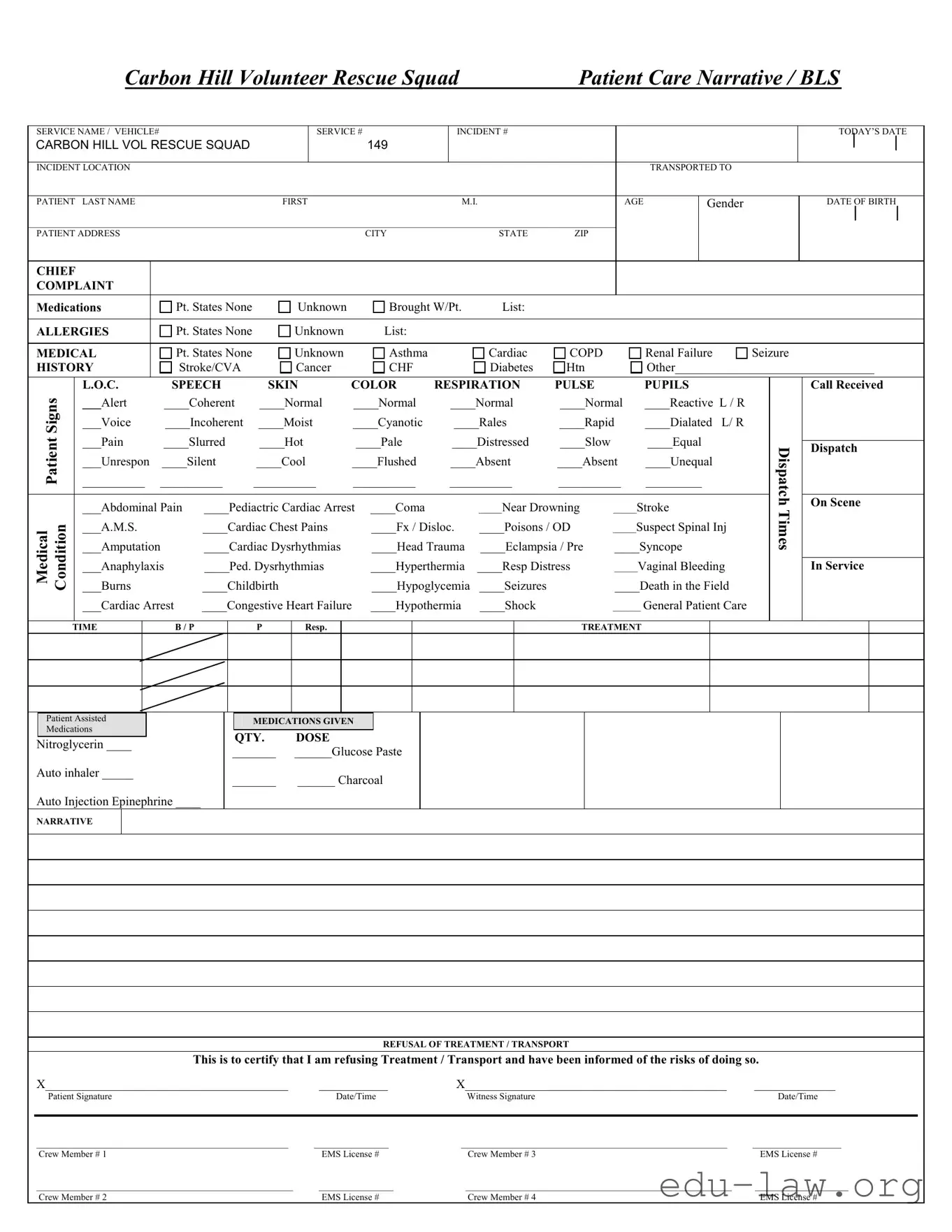
The Emergency Medical Services (EMS) Run Report is similar to the Patient Care Report form in that it documents the details of a medical incident. This report includes information such as the patient's demographics, the nature of the emergency, and the treatment provided. Just like the Patient Care Report, it serves to ensure continuity of care and provides critical information for future medical treatment.
The Incident Report is another document that shares similarities with the Patient Care Report. It captures the circumstances surrounding an emergency, including the time, location, and nature of the incident. While the Patient Care Report focuses more on patient care and treatment, the Incident Report highlights the overall context and response of emergency services, making both essential for comprehensive documentation.
The Medical History Form is a crucial document that resembles the Patient Care Report. It collects detailed information about a patient's past medical conditions, medications, and allergies. This form aids healthcare providers in understanding a patient's background, just as the Patient Care Report does during an emergency response.
The Consent for Treatment Form is also akin to the Patient Care Report. It requires patients to give permission for medical treatment, often including information about risks and benefits. This document is vital in ensuring that patients are informed, paralleling the Patient Care Report's emphasis on patient rights and informed consent.
The Transfer of Care Form is similar in purpose to the Patient Care Report, as it documents the handoff of a patient from one healthcare provider to another. This form ensures that all relevant information about the patient's condition and treatment is communicated effectively, just like the detailed accounts found in the Patient Care Report.
The Discharge Summary is another related document. It provides a comprehensive overview of a patient's treatment and condition at the time of discharge from a healthcare facility. Like the Patient Care Report, it includes critical information that can influence future care and treatment decisions.
The Trauma Assessment Form is closely related to the Patient Care Report, especially in emergency situations. It focuses specifically on trauma patients, documenting injuries, vital signs, and treatment provided. Both forms aim to ensure that healthcare providers have the necessary information to deliver appropriate care.
The Patient Transport Record is similar as it tracks the details of a patient during transport. This document includes information about the patient's condition, vital signs, and care provided en route to a medical facility. Like the Patient Care Report, it emphasizes the importance of continuous monitoring and documentation.
The Prescription Record is another document that shares similarities with the Patient Care Report. It details the medications prescribed to a patient, including dosages and instructions. This record is essential for ensuring that patients receive the correct medications, paralleling the Patient Care Report's focus on medication administration during emergencies.
Finally, the Follow-Up Care Plan is akin to the Patient Care Report in that it outlines the next steps in a patient's treatment after an emergency. This document includes recommendations for further care and monitoring, ensuring that patients receive ongoing support, much like the information recorded in the Patient Care Report.