What is the purpose of the Medication Count Sheet?
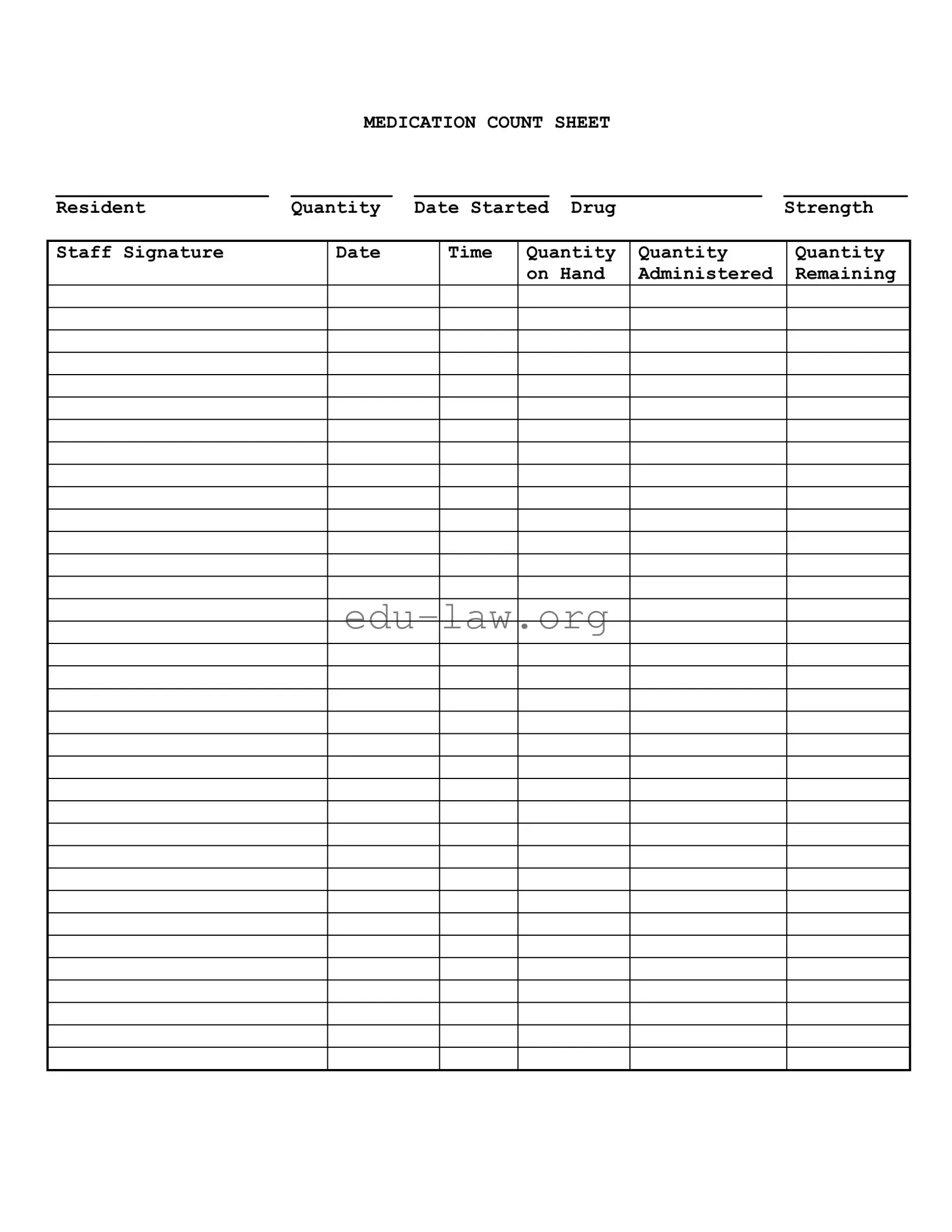
The Medication Count Sheet is a vital tool used in healthcare settings to track the administration of medications to residents. It helps ensure that the correct dosage is given at the right times, thereby enhancing patient safety. By documenting the quantity of medication on hand, the amount administered, and the remaining stock, healthcare staff can maintain accurate records and prevent medication errors.
How should the Medication Count Sheet be filled out?
To fill out the Medication Count Sheet, staff should start by entering the resident's name and the specific medication details, including the drug name, strength, and the date the medication was started. Each time medication is administered, the staff member must record the quantity given, the time of administration, and their signature. It is crucial to update the quantity on hand to reflect the new stock level after administration. This process ensures that everyone involved in the care of the resident has access to accurate information.
Why is it important to document the quantity of medication remaining?
Documenting the quantity of medication remaining is essential for several reasons. First, it helps prevent medication shortages and ensures that residents receive their prescribed treatments without interruption. Second, it aids in identifying discrepancies or potential theft of medications. Finally, maintaining an accurate count supports compliance with regulatory standards and enhances overall accountability within the healthcare team.
What should be done if there is a discrepancy in the medication count?
If a discrepancy is found in the medication count, it is crucial to take immediate action. Staff should double-check the records to confirm whether an error occurred during documentation. If the discrepancy persists, it should be reported to a supervisor or the designated medication management team. Investigating the cause of the discrepancy is essential to ensure that it does not compromise patient safety or lead to further issues.
Who is responsible for maintaining the Medication Count Sheet?
All healthcare staff involved in administering medications share the responsibility for maintaining the Medication Count Sheet. This includes nurses, pharmacists, and any other authorized personnel. Each individual must ensure that their entries are accurate and up to date. Regular audits may also be conducted to verify compliance and accuracy, reinforcing the importance of teamwork in medication management.