What is the Individual Service Plan (ISP) Wisconsin form?
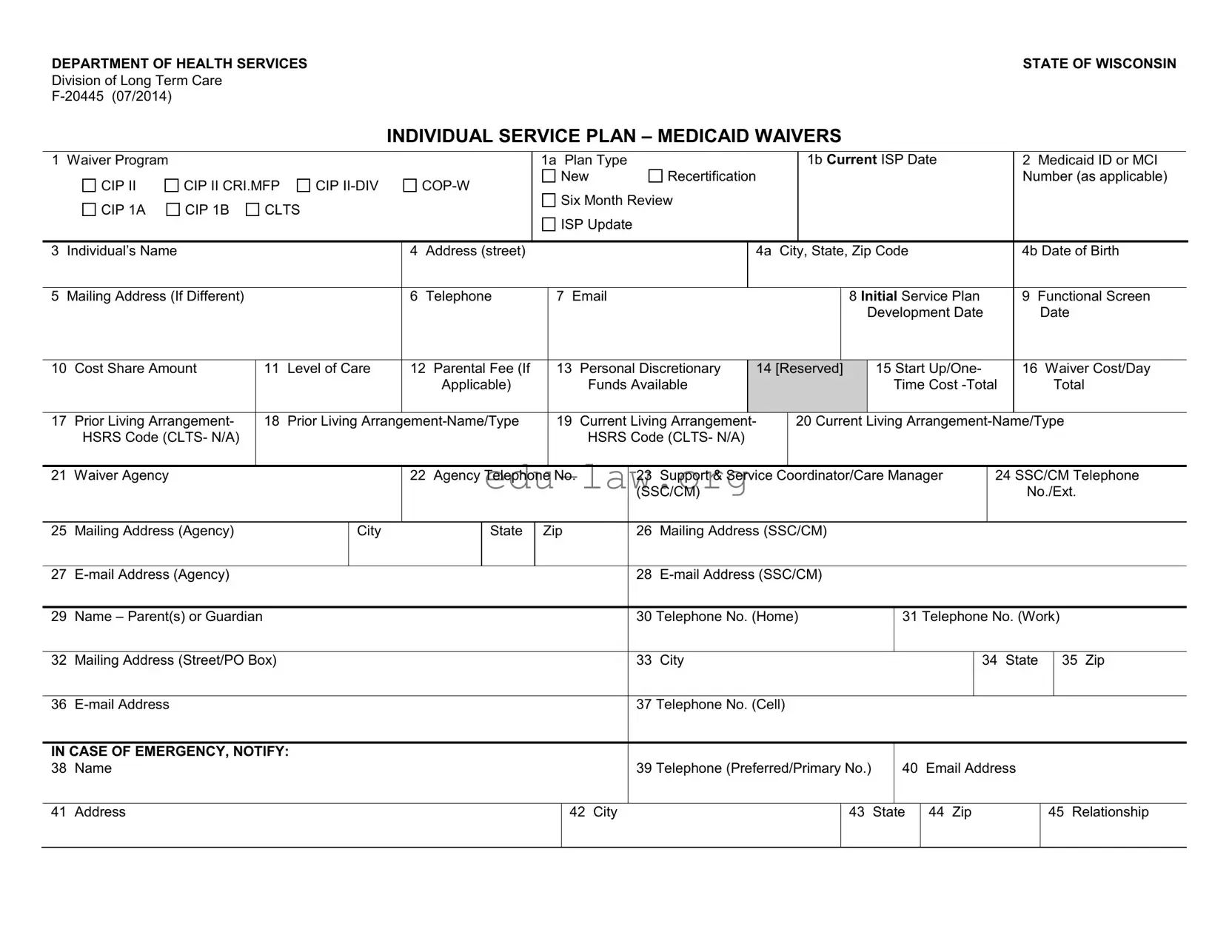
The Individual Service Plan (ISP) Wisconsin form is a document used to outline the services and supports needed for individuals enrolled in Medicaid waiver programs. It details the participant's needs, preferences, and the services they will receive to ensure their well-being and quality of life.
Who needs to complete the ISP form?
The ISP form must be completed for individuals who are applying for or are already enrolled in Medicaid Home and Community-Based Services (HCBS) programs. This includes participants in various waiver programs, such as CIP II, CLTS, and others.
What information is required on the ISP form?
The ISP form requires detailed information, including the individual's name, address, Medicaid ID, date of birth, current living arrangements, and contact information for the participant and their support coordinator. It also includes specific service codes, service providers, and details about the services being provided.
How often should the ISP be reviewed?
The ISP should be reviewed at least every six months. During this review, the participant or their guardian will discuss any changes in needs or services. If updates are necessary, they will be documented on the form.
What rights do participants have regarding their ISP?
Participants have the right to choose between various service options, including community services or institutional care. They can select from qualified providers and are informed of their rights and responsibilities within the Medicaid waiver programs. Participants also have the right to request a hearing if they disagree with decisions regarding their eligibility or services.
What happens if changes are needed in the ISP?
If changes are required, the support coordinator will work with the participant or guardian to update the ISP. This may involve adding, reducing, or changing the frequency of services. The updated information will be documented on the ISP form.
Who signs the ISP form?
The ISP form must be signed by the participant, their guardian or authorized representative, and the support and service coordinator. Witness signatures may also be required. These signatures indicate agreement with the content of the plan and the services to be provided.
What is the purpose of the cost share amount listed on the ISP?
The cost share amount reflects any financial contribution that the participant may need to make toward their care. This amount is determined based on the individual’s financial situation and is included in the ISP to ensure transparency regarding funding for services.
Where is the completed ISP form submitted?
The completed ISP form is submitted to the Department of Health Services (DHS) and copies are provided to the county care manager or support coordinator, the individual, and their authorized representative. This ensures that all parties involved have access to the most current service plan.