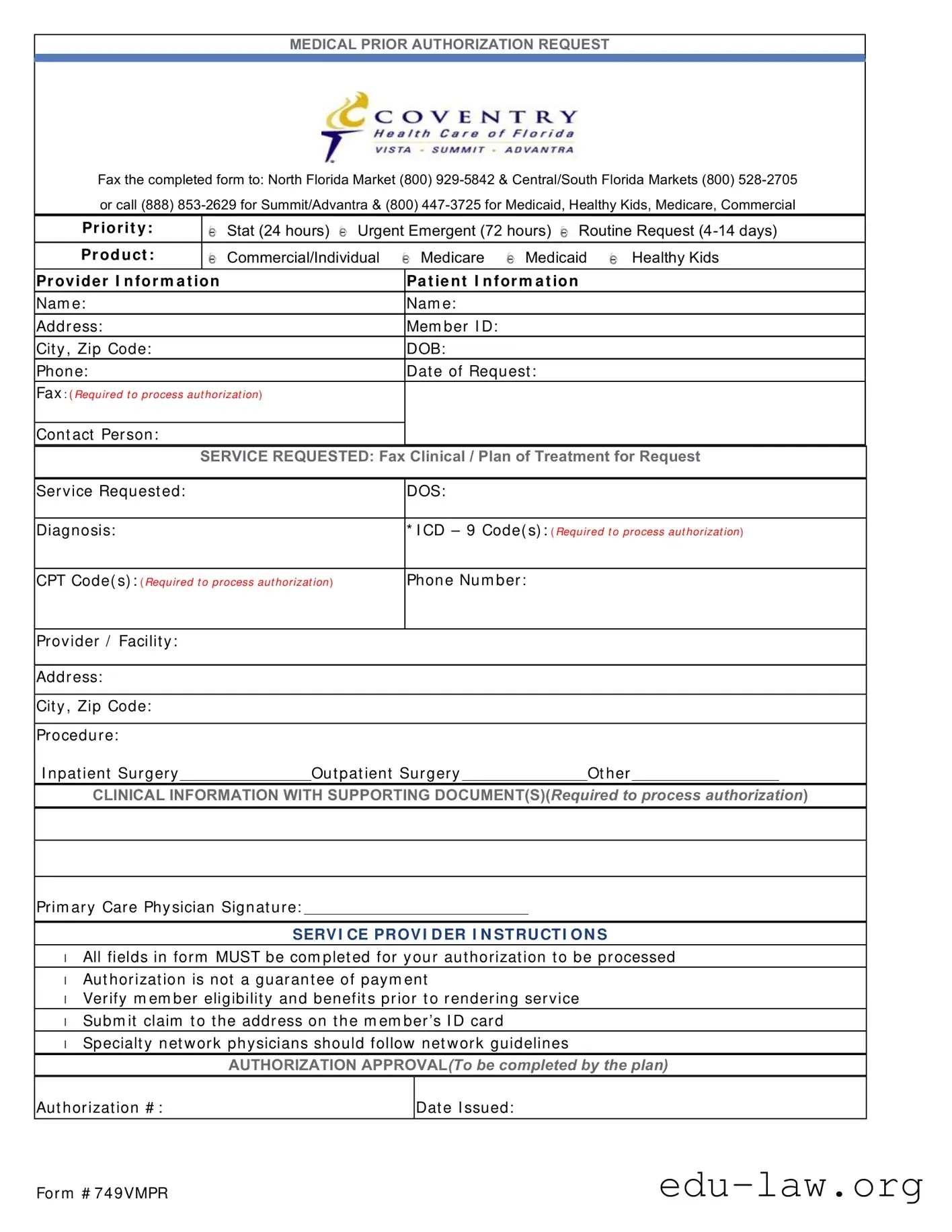
The Coventry Prior Authorization form shares similarities with the UnitedHealthcare Prior Authorization form. Both documents require detailed patient and provider information, including names, addresses, and contact numbers. Each form also necessitates the submission of specific clinical information and supporting documentation to process the authorization request. The urgency of the request can vary, with options for urgent or routine requests, similar to the categorizations found in the UnitedHealthcare form.
Another comparable document is the Aetna Prior Authorization form. Like the Coventry form, it requires comprehensive patient details, including the member ID and date of birth. Both forms emphasize the need for a clinical rationale for the requested service, necessitating the inclusion of relevant diagnosis and procedure codes. Additionally, both documents inform providers that authorization does not guarantee payment, highlighting the importance of verifying member eligibility beforehand.
The Cigna Prior Authorization form is also similar in structure and purpose. It requires the same essential information about the patient and provider. Both forms ask for diagnosis and procedure codes, ensuring that the request is supported by adequate clinical documentation. Cigna’s form, like Coventry’s, outlines the need for urgent or routine processing, making it clear how quickly the request needs to be addressed.
The Blue Cross Blue Shield (BCBS) Prior Authorization form exhibits similar features as well. It includes sections for patient and provider information, along with a requirement for clinical documentation. Both forms emphasize the importance of completing all fields to avoid delays in processing. Furthermore, BCBS also specifies that authorization does not guarantee payment, aligning with the messaging found in the Coventry form.
The Humana Prior Authorization form mirrors the Coventry form in its layout and required information. Both documents necessitate the submission of clinical details, including diagnosis and procedure codes. The urgency of the request is categorized in a similar manner, allowing providers to specify whether the request is routine, urgent, or emergent. This consistency helps streamline the authorization process across different insurance providers.
The Medicare Prior Authorization form also shares key similarities with the Coventry form. It requires detailed patient information, including member ID and date of birth, just as the Coventry form does. Both documents demand supporting clinical information to justify the service request. Moreover, they both highlight the need to verify eligibility before rendering services, ensuring that providers understand the importance of this step.
The Medicaid Prior Authorization form exhibits similar characteristics as well. It requires comprehensive patient and provider information, along with clinical details to support the authorization request. Both forms emphasize that the authorization process is not a guarantee of payment, which is crucial for providers to understand when planning patient care. Additionally, the forms both allow for categorizing the urgency of the request, which helps prioritize processing.
Finally, the Tricare Prior Authorization form shares common elements with the Coventry form. It requires essential information about the patient and provider, including contact details and member ID. Both documents necessitate the inclusion of diagnosis and procedure codes, ensuring that the request is adequately supported. Furthermore, both forms instruct providers to verify eligibility before services are rendered, emphasizing the importance of this step in the authorization process.