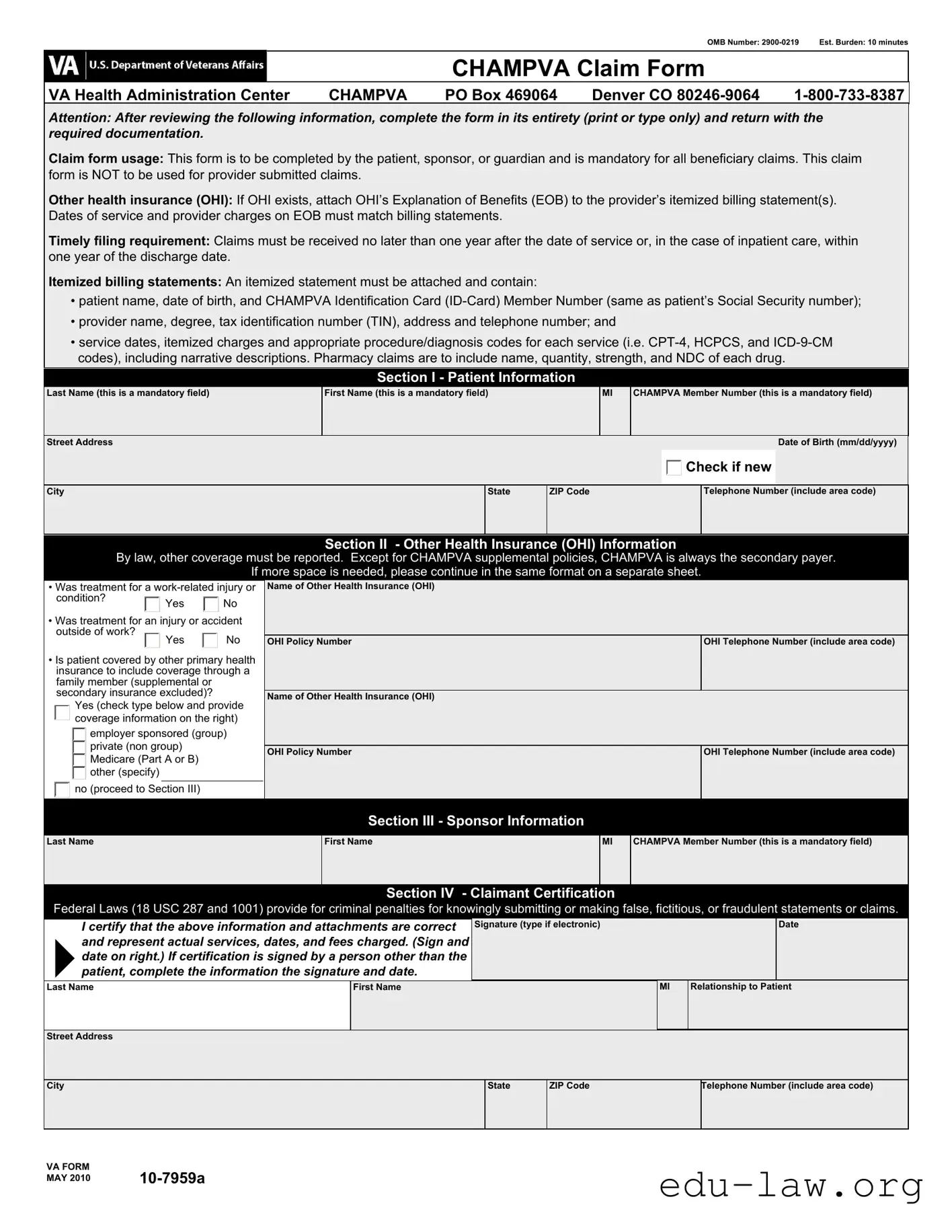
The CMS-1500 form, also known as the Health Insurance Claim Form, is widely used by healthcare providers to bill Medicare and other health insurers. Like the CHAMPVA Claim Form, it requires detailed patient information, including identification numbers and service dates. Both forms demand that itemized billing statements accompany the claim, ensuring that all charges are clearly documented. This helps streamline the claims process, allowing insurers to verify the services rendered and expedite payment.
The UB-04 form, or the Uniform Bill 04, is another essential document used for billing hospital services. Similar to the CHAMPVA form, it captures comprehensive information about the patient, provider, and services provided. Both forms require itemized charges and relevant codes to describe the services. While the CHAMPVA form is specific to veterans’ health care, the UB-04 is utilized by a broader range of healthcare facilities, making it a vital tool in the billing process.
The VA Form 10-10EZ is the application for health benefits for veterans. This document is similar to the CHAMPVA Claim Form in that it collects crucial patient information necessary for processing claims. Both forms serve to establish eligibility for benefits, although the 10-10EZ is focused on initial enrollment rather than claims submission. Proper completion of both forms is essential for ensuring that veterans receive the healthcare benefits they are entitled to.
The Medicare Part D Claim Form is used by beneficiaries to submit claims for prescription drug coverage. This form shares similarities with the CHAMPVA Claim Form in that both require detailed information about the medications dispensed and the associated costs. Additionally, both forms necessitate the inclusion of supporting documents, such as receipts or pharmacy statements, to validate the claims being submitted.
The Blue Cross Blue Shield Claim Form is utilized by members to file claims for covered medical services. Like the CHAMPVA Claim Form, it requires the patient’s personal information and details about the services rendered. Both forms also mandate the submission of itemized bills and other documentation to support the claim. This ensures that claims are processed accurately and efficiently, facilitating timely reimbursement for medical expenses.
The TRICARE Claim Form is designed for military families to submit health care claims. Similar to the CHAMPVA Claim Form, it collects patient and provider information and requires itemized billing statements. Both forms serve to verify the services provided and the associated costs, ensuring that beneficiaries receive the appropriate benefits. Timely submission of both forms is critical to avoid delays in processing claims.
The Health Insurance Marketplace Application is used to apply for health coverage under the Affordable Care Act. While it primarily serves a different purpose, it shares similarities with the CHAMPVA Claim Form in that it requires detailed personal and financial information to determine eligibility for benefits. Both forms aim to assist individuals in accessing necessary healthcare services, though they cater to different populations.
The Workers' Compensation Claim Form is used by employees to report work-related injuries and seek benefits. This form is similar to the CHAMPVA Claim Form in that it requires detailed information about the claimant and the circumstances surrounding the claim. Both forms emphasize the importance of accurate reporting and supporting documentation to ensure that claims are processed without unnecessary delays.
The Medicaid Claim Form is used by healthcare providers to bill for services provided to Medicaid beneficiaries. Like the CHAMPVA Claim Form, it requires detailed patient and service information, including itemized billing. Both forms are critical in ensuring that healthcare providers receive payment for the services rendered, facilitating access to care for individuals covered under these programs.